Normal hCG Levels in Early Pregnancy
Prenatal Testing
Obie Editorial Team

What is hCG?
hCG stands for human chorionic gonadotropin, the pregnancy hormone, which is produced by the placenta and detected in the blood within a few days after implantation. When you test at home with a pregnancy test, you actually test for the presence of hCG in the urine. If hCG is present, then the pregnancy test will be positive, and that means you are pregnant unless there is a false positive pregnancy test.
How does hCG increase during early pregnancy?
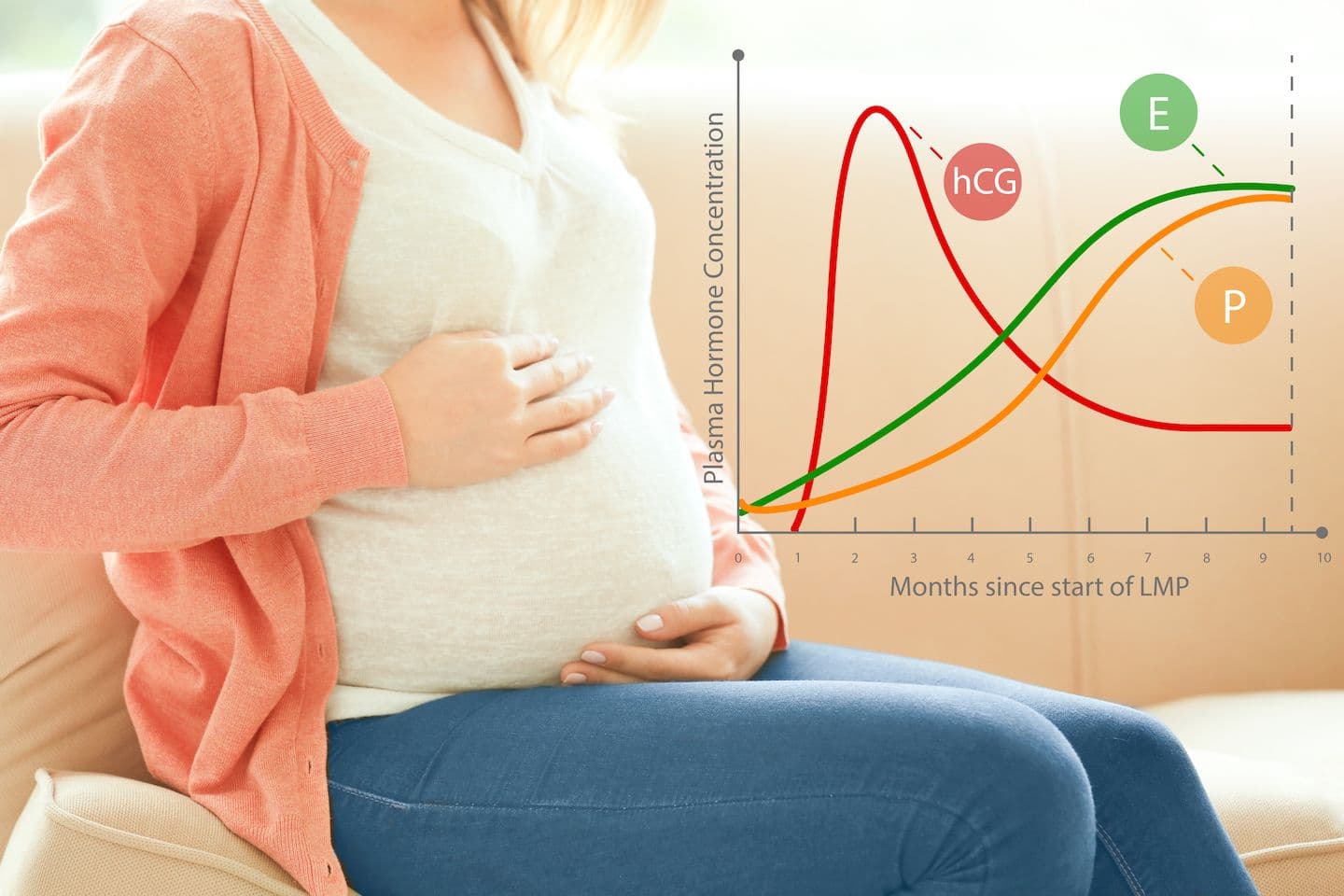
hCG usually doubles every 48-72 hours very early in pregnancy and every 3-4 days later on until about 9-10 weeks of the pregnancy when it levels off. There is no single "normal" hCG level during early pregnancy and there are wide ranges of normal levels that you can check with our hCG calculator.
What are normal hCG values and rise?
- Blood hCG under 5 mIU/ml: Negative. Not pregnant
- Blood hCG between 5-25 mIU/ml: "Equivocal". Maybe pregnant, maybe not. Repeat test in a couple of days
- Blood hCG over 25 mIU/ml: You are pregnant!
- One single hCG reading is not enough to make a clear diagnosis. Several hCG tests 2 or more days apart give a more accurate assessment of the situation.
- The blood hCG levels should not be used to date a pregnancy since these numbers can vary so widely.
- For postmenopausal women, an hCG level up to 14 mIU/ml can be considered normal.
- In a study of 20 patients in the first 40 days of pregnancy, the hCG concentration rose by at least 66 percent every 48 hours in 85 percent of viable IUPs; but still, 15 percent of viable pregnancies had a rate of hCG rise less than this threshold. (Kadar 1981)
- An increase of >=35% in 48 hours can still be considered normal (Seeber 2006; Morse 2012)
- hCG levels are best checked based on ovulation/fertilization day because the day of the last period can vary.
How does implantation affect hCG?
Implantation occurs on average, 9 days after ovulation (with a range of 6-12 days) or about 5 days before a missed period. hCG levels are detected in the blood as early as 2-3 days, and in the urine 3-4 days, after implantation. A urine pregnancy test would be expected to be positive around the time of a missed period or 14-15 days after implantation (which can be as early as several days before a missed period).
Find out what your levels mean with our hCG calculator!
What are good hCG levels in early pregnancy?
- In most normal pregnancies, at hCG levels below 1,200 mIU/ml, the hCG level usually doubles every 48-72 hours and normally increases by at least 60% every two days.
- In early pregnancy, a 48-hour increase of hCG by 35% can still be considered normal.
- As your pregnancy progresses, the hCG level increase slows down significantly.
- Between 1,200 and 6,000 mIU/ml serum, the hCG level usually takes 72-96 hours to double.
- Above 6,000 mIU/ml, the hCG level often takes over four or more days to double.
- In general, when the hCG level reaches 7200 mIU/ml, a yolk sac should be seen.
- At an hCG level greater than 10,800 mIU/ml, there should be a visible embryo with a heartbeat.
It makes little sense to follow the hCG values above 6,000 mIU/ml as the increase is normally slower and not related to how well the pregnancy is doing. After 10-12 weeks, the hCG level increase will slow even further and eventually will even decline before reaching a plateau for the duration of the pregnancy.
A normal hCG rise over several days prior to 6 weeks of the pregnancy usually indicates a viable pregnancy.
Can hCG levels tell you if your pregnancy is healthy?
Pregnancy blood hCG levels are not recommended for testing the viability of the pregnancy when the hCG level is well over 6,000 and/or after 6-7 weeks of the pregnancy. Blood hCG levels are useless for testing the viability of the pregnancy if the hCG level is well over 6,000 and/or after 6-7 weeks days of the pregnancy. In general, after 6-7 weeks the best indication of a healthy pregnancy is a good fetal heartbeat. Instead of the hCG, after 6 weeks or an hCG above 6,000 mIU/cc, the health of the pregnancy can best be confirmed with a sonogram to confirm the presence of a fetal heartbeat. Once a fetal heartbeat is seen, the hCG levels don't tell you much more about the pregnancy viability.
There is a wide range of normal hCG values and the values are different in blood serum or urine. Urine hCG levels are usually lower than serum (blood) hCG levels. There is no single normal human chorionic gonadotropin hCG level that always indicates a healthy pregnancy and there is a very wide range of human chorionic gonadotropin hCG levels values as the pregnancy progresses.
Read about slow-rising hCG levels.
Comparing slow rising and normal rising hCG levels
Comparing changes in hCG titers with those of established expected curves can help the doctor determine what to do about the pregnancy and how to counsel the patient. However, there are many limitations to the serial assessment of hCG titers and the titers should never be used exclusively to replace clinical judgment based on symptoms or signs.
A normally rising hCG level would usually be a level that rises over 60% over a 48 period, though later on in pregnancy, the rise would be normally slower. Seebert et al reported in 2006 and Morse confirmed in 2012 that a rise of at least 35% over 48 hours was proposed as the minimal rise consistent with a viable intrauterine pregnancy.
Does a fast-rising hCG signal twins?
You cannot diagnose a twin pregnancy just from the hCG. There is no sufficient scientific evidence that with twins there is always a faster-than-usual rise in hCG. Normal hCG values can vary up to 20 times in normal pregnancies. Variations in hCG increases are not necessarily a sign that the pregnancy is abnormal or that there are two or more fetuses.
Normal amount of serum hCG levels by weeks
3 weeks: 5-50 mIU/cc
4 weeks: 4-426 mIU/cc
5 weeks: 19-7,340 mIU/cc
6 weeks: 1,080-56,500 mIU/cc
7 - 8 weeks: 7,650-229,000 mIU/cc
9 - 12 weeks: 25,700-288,000 mIU/cc
13 - 16 weeks: 13,300-254,000 mIU/cc
17 - 24 weeks: 4,060-165,400 mIU/cc
25 - 40 weeks: 3,640-117,000 mIU/cc
Sources:
Barnhart KT, Sammel MD, Rinaudo PF, et al. Symptomatic patients with an early viable intrauterine pregnancy: HCG curves redefined. Obstet Gynecol 2004; 104:50.
Silva C, Sammel MD, Zhou L, et al. Human chorionic gonadotropin profile for women with ectopic pregnancy. Obstet Gynecol 2006; 107:605.
Kadar N, Caldwell BV, Romero R. A method of screening for ectopic pregnancy and its indications. Obstet Gynecol 1981; 58:162.
Seeber BE, Sammel MD, Guo W, et al. Application of redefined human chorionic gonadotropin curves for the diagnosis of women at risk for ectopic pregnancy. Fertil Steril 2006; 86:454.
Morse CB, Sammel MD, Shaunik A, et al. Performance of human chorionic gonadotropin curves in women at risk for ectopic pregnancy: exceptions to the rules. Fertil Steril 2012; 97:101.
Kadar N, DeVore G, Romero R. Discriminatory hCG zone: its use in the sonographic evaluation for ectopic pregnancy. Obstet Gynecol 1981; 58:156.
Read More