Slow Rising hCG Levels: What It Means for Pregnancy
Pregnancy
Obie Editorial Team

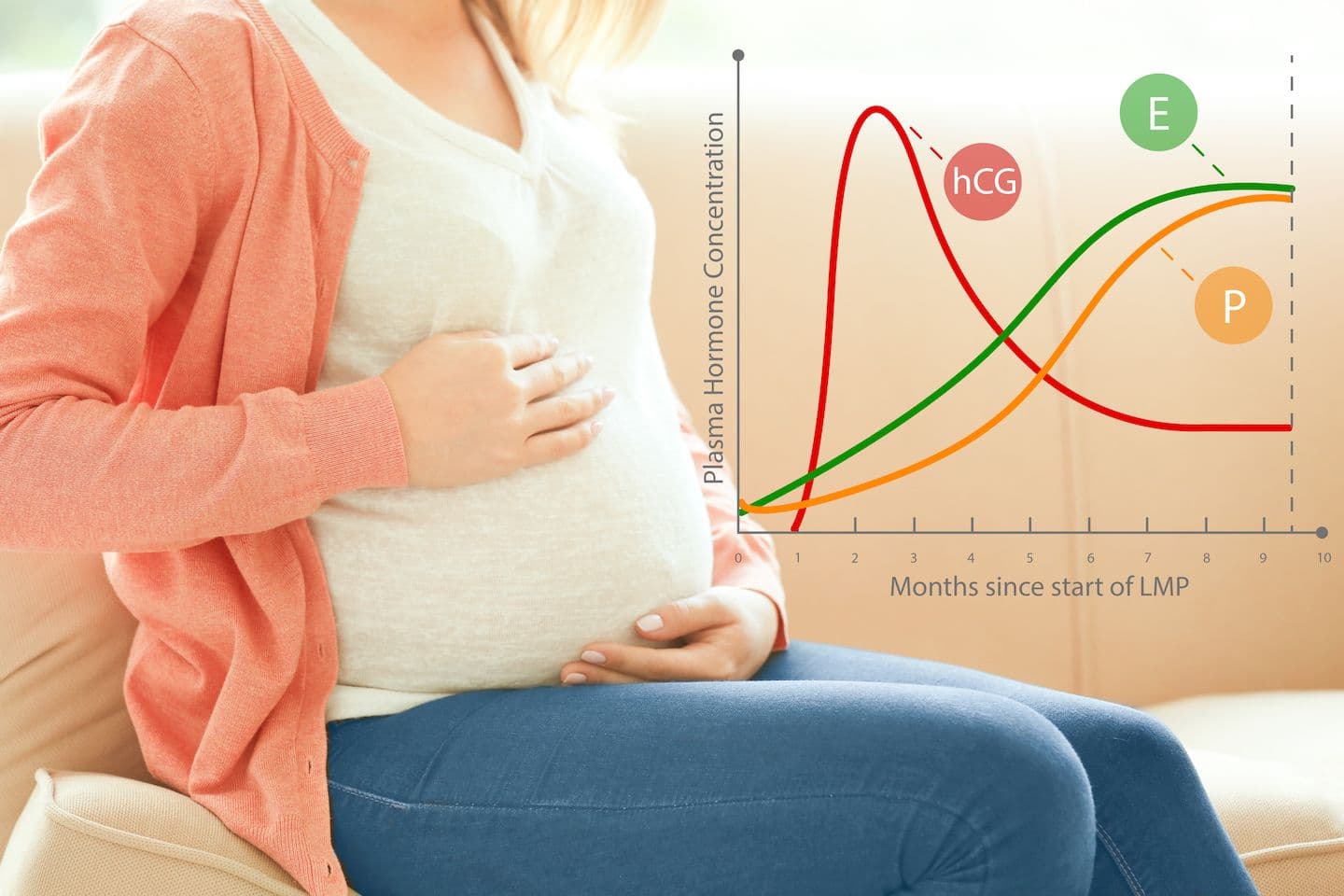
hCG Levels in Early Pregnancy
hCG usually doubles every 48-72 hours very early in pregnancy, when the hCG is below 6,000 mIU/ml. A rise above 35% in 48 hours is still considered normal and a rise below 35% in 48 hours is generally considered abnormal.
Blood hCG levels are not very helpful to test for the viability of the pregnancy if the hCG level is above 6,000 and/or after 6-7 weeks of the pregnancy. Instead, to test the health of the pregnancy better, a sonogram should be done to confirm the presence of a fetal heartbeat. Once a fetal heartbeat is seen, it is not recommended to check the pregnancy viability with hCG levels.
The measurement of serum hCG concentrations over several days, usually 48-72 hours apart is important to identify a normal from an abnormal early pregnancy. This is usually done before an ultrasound can be of value to assess the viability of the pregnancy.
Decreasing hCG Levels
When the hCG level is decreasing early in pregnancy, it is clear that the pregnancy is not viable, but after 10-11 weeks a decrease is not unusual in normal pregnancies. The management of cases with too low or decreasing hCG levels often consists of observation or intervention. The rate of decline associated with nonviable pregnancies that resolved with expectant management has been described, with a faster decline observed with higher hCG levels at presentation. A rate of decline that is slower than 21 to 35% in 48 hours suggests the presence of retained trophoblastic tissue or ectopic pregnancy and indicates the need for intervention to achieve a definitive diagnosis.
Expected minimum % decline in serum HCG in nonviable pregnancies
| Initial hCG (MIU/ml) | % Decline after 2 days | % Decline after 4 days | |
| 50 | 12% | 26% | |
| 150 | 18% | 39% | |
| 250 | 21% | 44% | |
| 500 | 24% | 50% | |
| 1000 | 28% | 55% | |
| 2000 | 31% | 60% | |
| 2500 | 32% | 62% | |
There is no single "normal" hCG level in early pregnancy.
Seebert et al reported in 2006 and Morse confirmed this in 2012 that a rise of at least 35% over 48 hours was proposed as the minimal rise consistent with a viable early intrauterine pregnancy. So it would be wrong to always assume the presence of a nonviable pregnancy even if there is an hCG rise below 53% over 48 hours during the first 4 weeks of the pregnancy. There is usually a range of hCG levels in normal pregnancy which you can check with our hCG calculator.
Comparing slow rising and normal rising hCG levels
Comparing changes in hCG titers with those of established expected curves can help the doctor determine what to do about the pregnancy and how to counsel the patient. However, there are many limitations to the serial assessment of hCG titers and the titers should never be used exclusively to replace clinical judgment based on symptoms or signs.
Slow rising hCG levels could be associated with:
- A normal pregnancy
- A miscarriage
- An ectopic pregnancy
Only your doctor can determine what it could be more likely.
Sources:
Chart adapted from Barnhart et al., Ob Gyn 2004 (9); and Chung et al., Fertil Steril 2006 (10) Seeber, hCG in early pregnancy. Fertil Steril 2012
Read More