Artificial Intrauterine Insemination (IUI)
Infertility
Obie Editorial Team
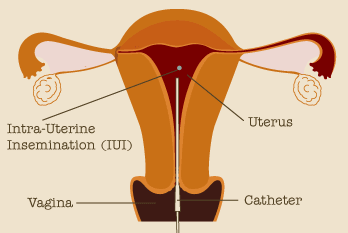
What is intrauterine insemination?
Intrauterine insemination is also known as artificial insemination or IUI. Human artificial insemination with sperm was first used in the 1940s. The IUI procedure can be an effective treatment for some causes of infertility and is also used for other reasons, such as in some LGBTQ pregnancies and/or for pregnancy without a partner.
When is IUI used?
IUI is most commonly used for unexplained infertility but can also be performed in other circumstances such as:
- Mild endometriosis
- Problems with ovulation
- Male factor infertility
- Cervical factor infertility
- Hostile cervix
- Ejaculation issues
- When there is a sperm donor
- Semen allergy
- No partner available who produces sperm
- When penetration by a penis is not desired.
However, IUI is not effective for couples with:
- Tubal blockage or severe tubal damage
- Ovarian failure (menopause)
- Severe male factor infertility
- Advanced stages of endometriosis
Female age and a reduced ovarian reserve are significant factors with IUI and intrauterine insemination has a lesser chance of working in:
- Women over 40
- Significantly elevated day 3 FSH level
- Significantly reduced ovarian reserve
If the sperm count, motility, and morphology scores are low, intrauterine insemination is unlikely to work (see the table with male factor IUI success rates at the bottom of this page). With significant male factor issues, IVF with ICSI is indicated and has a higher success rate for women under age 40.
Insemination is a reasonable initial treatment that should be utilized for a maximum of 3-4 months in women who are ovulating on their own. It is reasonable to try IUI for longer than this in women with polycystic ovaries (PCOS) and those who have trouble ovulating and have been given drugs to ovulate.
How does the IUI procedure take place?
- The woman usually is given medications to stimulate the development of multiple eggs and the insemination is timed to coincide with ovulation.
- A semen specimen is either produced at home or in the office by masturbation after 2-5 days of abstinence from ejaculation or semen is purchased.
- The semen is "washed" in the laboratory (called sperm processing or sperm washing). The sperm is separated from the other components of the semen and concentrated in a small volume. Various media and techniques can be used for washing and separation. Sperm processing takes about 30-60 minutes.
- A speculum is placed in the vagina and the cervical area is gently cleaned.
- The washed specimen of highly motile sperm is placed either in the cervix (intracervical insemination, ICI) or higher in the uterine cavity (intrauterine insemination, IUI) using a sterile, flexible catheter.
Timing of intrauterine insemination (IUI)
The timing of the IUI usually depends on when ovulation is expected, usually within 24-36 hours prior to ovulation. It also depends on whether the cycle is a natural cycle, without medications to induce ovulation, or a cycle with medications to induce ovulation and a cycle with a "trigger shot", an hCG shot after which ovulation usually happens 36 hours later.
How successful is intrauterine insemination (IUI)?
The success rate of IUI depends on why it's being done, but in general, it's similar to the natural monthly pregnancy rate of 15-20% per month but also depending on the sperm count:
Single versus double intrauterine insemination (IUI)
Single IUI is one IUI procedure between 12 to 36 hours before ovulation. There is no consistent agreement as to how many hours are optimal. A double IUI is when there are two IUI procedures, such as one IUI at 36 hours and another IUI at 12 hours before presumed ovulation. Studies have been done to see if double IUI has a higher pregnancy rate. At the present time, there is insufficient evidence to support the use of double IUI in clinical practice.
Is there pain and intrauterine insemination?
The intrauterine insemination procedure, if done properly, is associated with little or no discomfort. Most clinics let you remain laying down for a few minutes after the procedure, although it has not been shown to improve success rates. The sperm has been put above the vagina and cervix, so it will not leak out when you stand up.







