Testing and Interpreting Measures of Ovarian Reserve
Infertility Tests
Obie Editorial Team
Testing and Interpreting Measures of Ovarian Reserve: A Committee Opinion
Practice Committee of the American Society for Reproductive Medicine
Fertil Steril. 2015;103:e9-e17
Currently, there is no uniformly accepted definition of decreased ovarian reserve (DOR), as the term may refer to three related but distinctly different outcomes: oocyte quality, oocyte quantity, or reproductive potential. Available evidence concerning the performance of ovarian reserve tests is limited by small sample sizes, heterogeneity among study design, analyses and outcomes, and the lack of validated outcome measures.
Background
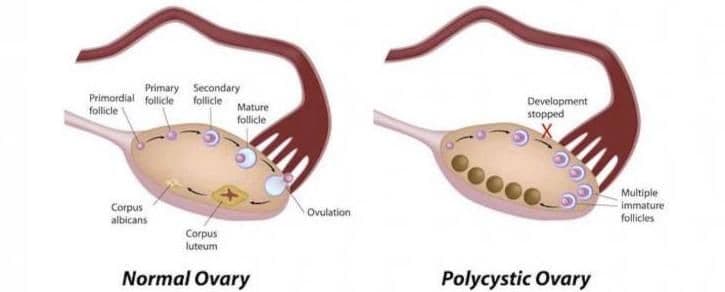
The peak number of ovarian follicles is reached by 18-20 weeks in utero, and from that point on, the number of follicles declines until menopause. The rate of decline is mostly genetically determined and is not influenced by pregnancy, lactation, or contraceptive pill use. Most of the follicles are actually lost by the time a woman enters her reproductive period at menarche. Ovarian surgery, chemotherapy, radiation therapy, or any injury to the vascular supply of the ovaries may expedite the loss. In addition, certain genetic mutations (45 XO, FMR1 mutations) are associated with a faster loss rate.
Follicles grow in waves, and it takes at least 3 months for a primordial follicle to reach ovulation. The final growth of the follicles is regulated by various hormones and depends on the interaction between the ovaries and the pituitary. It is during these last 2 weeks that the follicle destined to ovulate is selected and progresses to ovulation.
Because of a trend in couples delaying childbirth,, it's important that we discuss with women the age-related decline in fertility and quality of oocytes. This committee opinion evaluated the advantages and disadvantages of certain tests to estimate ovarian reserve and discusses their interpretation.
The Paper
The paper first explores what ovarian reserve is and concludes that it is the assessment of the number and quality of a woman's oocytes. Ovarian reserve testing is typically done with the aim of predicting reproductive potential and when menopause can be expected.
There are various tests that can be used to evaluate ovarian capacity:
• Follicle-stimulating hormone (FSH) is the primary stimulus for final follicle maturation. FSH is under the negative feedback of estradiol and inhibin B. Inhibin B depends on the number of follicles in the ovaries. As the number of follicles declines, inhibin B will be reduced as well, and FSH becomes less suppressed. Therefore, elevated FSH indicates diminished follicle pool. While an elevated FSH is a reasonably good tool to predict poor response, it is only weakly associated with nonpregnancy. Proposed cut-off values in the literature vary widely, and lack of pregnancy can be reasonably predicted by very high values (>18-20 IU/L) that are rare in the infertile population. High FSH is not associated with an increased risk for aneuploidy. FSH is affected by significant cycle-to-cycle variability, but repeating the FSH to wait for a "good" cycle has not been shown to improve outcome. High early-follicular-phase estradiol indicates fast follicle development and can be seen when the follicle pool is small. The test, however, is not predictive enough to identify poor responder patients.
• Clomiphene citrate challenge test is a dynamic test of ovarian function. Among those with a low reserve, the FSH value will be elevated after exposure to 5 days of 100 mg clomiphene citrate. This test, however, does not improve the accuracy of baseline FSH or antral follicle count and, therefore, should not replace them.
• Antimüllerian hormone (AMH) is a peptide that is also produced by the small follicles. It is fairly stable during the cycle and is associated with low intercycle variability. Low AMH values show good correlation with poor response during fertility treatment but have limited value in predicting nonpregnancy.
• Antral follicle count (AFC) is the sum of 2- to 10-mm follicles in the two ovaries. AFC is associated with limited intercycle variability, but there could be significant interobserver variability due to differences in experience or ultrasound quality. Low values (<7) are associated with poor response to stimulation. As with AMH, its predictive ability for pregnancy is limited.
The committee opinion does not recommend testing inhibin B as an ovarian function marker. Furthermore, according to this report, the combination of markers does not consistently improve the accuracy of testing.
The authors concluded that while there are multiple tests available to assess the follicle pool in the ovaries, the results should not be used to exclude patients from assisted reproductive technology (ART) treatments.
Viewpoint
There could be many potential indications to assess the size of the follicle pool in the ovaries. Such information would be useful for patients trying to determine when to start a family, for example. It also would be useful if a woman could predict how soon to expect menopause. In addition, medical treatments that affect ovarian reserve and their impact could be followed by assessing ovarian reserve. Patients who require some form of ART to achieve a pregnancy would like to know how likely the treatment is to succeed. Unfortunately, the available tests are not particularly useful when we try to address these problems.
What can we use these tests for, then? Patients who need ART will first undergo a stimulation to recruit several oocytes. For optimal results, we should aim for 10-15 oocytes. Not all patients, however, react the same to stimulation. Ovarian reserve markers could be useful to predict poor or hyper-response fairly accurately. The tests can be used to group patients as expected poor, normal, or hyper-responders, and the stimulation protocol and amount of gonadotropin for stimulation would be selected accordingly.
Assessment of ovarian function should be part of the evaluation of an infertile couple. While extreme values will not always rule out the possibility of pregnancy with ART, they are associated with the very low likelihood of success. Therefore, very low AMH or AFC values or very high FSH values can be used to discuss the extremely low chance of pregnancy. Patients can be counseled about alternative treatment options such as egg donation and can be advised against repetitive treatments.
In interpreting these test results, it's important to also consider age. A poor value in a young woman is more likely to indicate few but potentially good quality eggs and, therefore, a reasonably good chance for pregnancy. The same low value in an older woman, however, means few and poor quality eggs and, therefore, a very low chance to succeed.
References
- Gougeon A. Regulation of follicular ovarian development in primates: facts and hypotheses. Endocr Rev. 1996;17:121-155.
- Tremellen K, Savulescu J. Ovarian reserve screening: a scientific and ethical analysis. Hum Reprod. 2014;29:2606-2614.
- van der Gaast MH, Eijkemans MJ, van der Net JB, et al. Optimum number of oocytes for a successful first IVF treatment cycle. Reprod Biomed Online. 2006;13:476-480.
- Sunkara SK, Rittenberg V, Raine-Fenning N, Bhattacharya S, Zamora J, Coomarasamy A. Association between the number of eggs and live birth in IVF treatment: an analysis of 400 135 treatment cycles. Hum Reprod. 2011;26:1768-1774.
- Broekmans FJ, Kwee J, Hendriks DJ, Mol BW, Lambalk CB. A systematic review of tests predicting ovarian reserve and IVF outcome. Hum Reprod Update. 2006;12:685-718.
- Broer SL, Dólleman M, Opmeer BC, Fauser BC, Mol BW, Broekmans FJ. AMH and AFC as predictors of excessive response in controlled ovarian hyperstimulation: a meta-analysis. Hum Reprod Update. 2011;17:46-54.
- Nelson SM, Yates RW, Lyall H, et al. Anti-Müllerian hormone-based approach to controlled ovarian stimulation for assisted conception. Hum Reprod. 2009;24:867-875.
- van Rooij IA, Bancsi LF, Broekmans FJ, Looman CW, Habbema JD, te Velde ER. Women older than 40 years of age and those with elevated follicle-stimulating hormone levels differ in poor response rate and embryo quality in vitro fertilization. Fertil Steril. 2003;79:482-488.
Read More