What Is Polycystic Ovary Syndrome (PCOS)?
Reproductive Health2
Obie Editorial Team
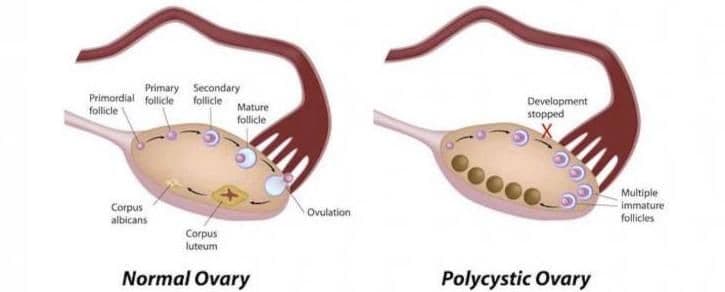
Polycystic ovary syndrome (PCOS) is the most common hormonal reproductive problem in women of childbearing age. PCOS is a health problem that can affect a woman’s menstrual cycle, hormones, insulin production, heart, blood vessels, and appearance — and it can cause infertility. PCOS is diagnosed in about 5-10 percent of women of childbearing age and is the leading cause of women with irregular periods and little or no ovulation.
What are the symptoms of PCOS?
Women who have PCOS may have typical symptoms but they also may not have any at all. PCOS often goes undiagnosed until women start trying to get pregnant and encounter difficulty. Many women have only a few symptoms while others have a multitude of symptoms, such as:
- Metabolic syndrome
- Infrequent menstrual periods, no menstrual periods, and/or irregular bleeding
- Infertility or inability to get pregnant because of not ovulating
- Hirsutism (excessive hair growth on the face, chest, abdomen, etc.)
- Hair loss (androgenic alopecia, in a classic "male baldness" pattern)
- Skin problems, such as acne, oily skin, dark skin patches, or skin tag
- Polycystic ovaries
- Increased levels of male hormones (hyperandrogenism)
- Weight gain or obesity, usually carrying extra weight around the waist
- Pelvic pain
- Insulin resistance
- Diabetes
- High blood pressure
- Lipid abnormalities, high cholesterol
- Increased growth of hair on the face, chest, stomach, back, thumbs, or toes
- Type 2 diabetes
- Patches of thickened and dark brown or black skin on the neck, arms, breasts, or thighs
- Sleep apnea, excessive snoring, and breathing stops at times while asleep
What causes PCOS?
No one knows the exact cause of PCOS. Women with PCOS frequently have a mother or sister with PCOS. However, there is not enough evidence to show a genetic link to this disorder. Many women with PCOS have a weight problem. Researchers are looking at the relationship between PCOS and the body’s ability to make insulin. Insulin is a hormone that regulates the change of sugar, starches, and other food into energy for the body’s use or storage. Since some women with PCOS make too much insulin, the ovaries may react by making too many male hormones, called androgens. This can lead to acne, excessive hair growth, weight gain, and ovulation problems.
How to find out if you have PCOS: The Rotterdam criteria
There is no single test to diagnose PCOS. Your doctor will take a medical history, perform a physical exam, possibly including an ultrasound, check your hormone levels, and measure glucose, or sugar levels, in the blood.
The most widely accepted criteria for diagnosing PCOS are the Rotterdam criteria. To make the diagnosis with the Rotterdam criteria, two of the following three criteria are required:
- oligo/anovulation
- polycystic ovaries on ultrasound
- Hyperandrogenism: clinical (hirsutism or less commonly male pattern alopecia) or
biochemical (raised FAI or free testosterone)
In addition, tests must be done to exclude other etiologies such as congenital adrenal hyperplasia, androgen-secreting tumors, Cushing syndrome, thyroid dysfunction, and hyperprolactinemia.
At the physical exam, the doctor will want to evaluate the areas of increased hair growth, so try to allow the natural hair growth for a few days before the visit. During a pelvic exam, the ovaries may be enlarged or swollen by the increased number of small cysts. This can be seen more easily by vaginal ultrasound, or screening, to examine the ovaries for cysts and the endometrium (the lining of the uterus). The uterine lining may become thicker if there has not been a regular period.
What are the treatments for PCOS?
Treatments are based on the symptoms each patient is having and whether she wants to conceive or needs contraception. Here are some treatment for managing PCOS:
Birth control pills:
For women who don’t want to become pregnant, birth control pills can regulate menstrual cycles, reduce male hormone levels, and help to clear acne. However, the birth control pill does not cure PCOS. The menstrual cycle will become abnormal again if the pill is stopped. Women may also think about taking a pill that only has progesterone, like Provera, to regulate the menstrual cycle and prevent endometrial problems, but progesterone alone does not help reduce acne and hair growth.
Diabetes medication:
Metformin, also called Glucophage, is an oral medication that is used to treat type 2 diabetes. It has been used to treat PCOS symptoms. Metformin affects the way insulin regulates glucose and decreases testosterone production. Abnormal hair growth will slow down and ovulation may return after a few months of use.
Fertility medication:
The main fertility problem for women with PCOS is the lack of ovulation. However, before beginning fertility medication, a woman should have her partner's sperm count checked and her tubes evaluated to make sure they are open. Clomiphene (pills) and Gonadotropins (shots) can be used to stimulate the ovaries to ovulate. PCOS patients are at increased risk for multiple births when using these medications. In-vitro Fertilization (IVF) is sometimes recommended to control the chance of having triplets or more. Metformin can be taken with fertility medications and helps to induce ovulation on lower doses of medication.
Medicine for increased hair growth/extra male hormones:
If a woman is not trying to get pregnant, some other medicines may reduce hair growth. Spironolactone is a blood pressure medicine that has been shown to decrease the male hormone’s effect on hair. Propecia, a medicine taken by men for hair loss, is another medication that blocks this effect. Both of these medicines can affect the development of a male fetus and should not be taken if pregnancy is possible. Other non-medical treatments such as electrolysis or laser hair removal are effective at getting rid of hair. A woman with PCOS can also take hormonal treatment to keep new hair from growing.
Surgery for PCOS:
Although it is not recommended as the first course of treatment, a surgery called ovarian drilling is available to induce ovulation. The doctor makes a very small incision above or below the navel and inserts a small instrument that acts like a telescope into the abdomen. This is called a laparoscopy. The doctor then punctures the ovary with a small needle carrying an electric current to destroy a small portion of the ovary. This procedure carries a risk of developing scar tissue on the ovary. This surgery can lower male hormone levels and help with ovulation. But these effects may only last a few months. This treatment doesn't help with increased hair growth and loss of scalp hair.
A healthy weight for PCOS
Maintaining a healthy weight is another way women can help manage PCOS. Since obesity is common with PCOS, a healthy diet and physical activity help maintain a healthy weight. This will help the body lower glucose levels, use insulin more efficiently, and may help restore a normal period. Even a loss of 10% of her body weight can help make a woman's cycle more regular.
How to get pregnant with PCOS
Getting pregnant with PCOS usually yields a higher success rate than other infertility conditions. The inability to get pregnant in most women with PCOS is usually the consequence of amenorrhea, the absence of ovulation. Anovulation may not be the only reason for many of these problems but you need to ovulate to get pregnant. Seeing an infertility specialist, an REI, or a reproductive endocrinologist will improve your chances of getting pregnant.
Lifestyle changes
With PCOS, losing weight can often help you to ovulate. The optimal BMI is between 20 and 25. Your doctor may recommend that you try losing weight first before trying any medications to see if ovulation and your fertility returns and whether pregnancy can occur naturally. Also, being at your optimal weight improves your chances of having a healthy pregnancy and a healthy baby once you do get pregnant.
Medications for getting pregnant with PCOS
The most common treatment for PCOS is Clomid. The American College of Obstetricians and Gynecologists (ACOG) recommends that clomiphene should be the primary medication for PCOS patients with infertility. Clomiphene indirectly causes eggs to mature and be released. One in 10 women who conceive with the aid of clomiphene will have multiple pregnancies, most commonly twins.
- Metformin may also be used alone or together with clomiphene to increase or regulate ovulation in women with PCOS.
- Letrozole slows estrogen production and causes the body to make more follicle-stimulating hormone (FSH), a hormone needed for ovulation. It is as effective as clomiphene in causing ovulation. Studies of letrozole in animals have shown that it causes birth defects if used during pregnancy, but there have been no studies of this drug in pregnant women.
- Gonadotropins are given as an injection and cause ovulation. Gonadotropins have a higher risk of multiple pregnancies than does treatment with clomiphene.
IVF for PCOS
IVF is usually effective in helping women with PCOS get pregnant. With IVF, sperm and an egg are placed in a dish outside the body. The sperm joins with the egg or your doctor helps this process with ICSI intracytoplasmic sperm injection. The fertilized egg is then placed inside the uterus. IVF offers women with PCOS the best chance of getting pregnant. There is more control of lessening the risk of multiple births, but it can be expensive and may not be covered by healthcare insurance.
Pregnancy and PCOS
Patients with PCOS are happy when they get pregnant, but just getting pregnant is not the end of complications. There appear to be several pregnancy complications in patients with PCOS:
- Cardiovascular complications such as:
- Postpartum strokes,
- Eclampsia
- Peripartum cardiomypathy
- Postpartum depression syndrome
- Miscarriage
- Gestational diabetes
- Pregnancy-induced high blood pressure
- Premature delivery
Researchers are studying how to prevent or reduce the chance of having these problems while pregnant, in addition to looking at how drugs like Metformin lower male hormone levels and limit weight gain in women who are obese when they get pregnant.
Read More









