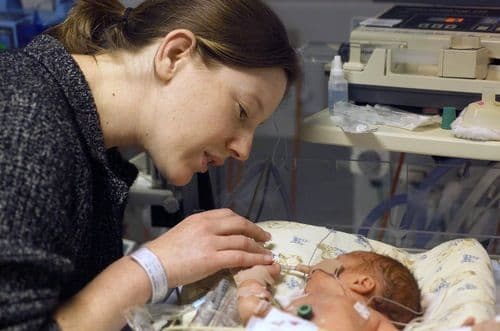
New Blood Test Identifies High-Risk Preemies
Pregnancy News
Obie Editorial Team
By Sandy Hemphill, Contributing Writer, BabyMed
Babies can have a tough time when born early but a new blood test developed by researchers at the University of Missouri (UM) identifies high-risk preemies so they can be carefully monitored to minimize certain life-threatening complications. The test detects white blood cells (eosinophilia) in the bloodstreams of preemies with necrotizing enterocolitis (NEC).
Necrotizing Enterocolitis
Necrotizing enterocolitis (death of bowel tissue) develops after a baby is born and is the second most common cause of death in babies born prematurely; the condition is almost always limited to preemies. The condition does not begin immediately after birth; babies born the most premature usually develop symptoms later than preemies born closer to term.
In some cases, NEC can be successfully treated without surgery but more severe cases and cases in which complications develop can require extensive medical interventions, including hospitalization that may last a year.
Eosinophilia
White blood cells in the blood indicate the presence of allergy or infection. Eosinophilia, one of five specific types of white blood cells, compose only about 2% to 4% of the white blood cells in the bloodstream but are more concentrated in the mucous membranes that line the digestive, lower urinary, and respiratory tracts.
Elevated levels of eosinophils in the blood of preemies with NEC signal the early development of complications. The UM study found that NEC complications were associated with a sustained blood eosinophilia count of 5% or greater. Early detection of elevated eosinophilia alerts the neonatal intensive care (NICU) team to be especially vigilant in monitoring the baby’s health and maintain a heightened awareness of any sign of disease escalation.
The UM research team discovered that preemies most likely to test positive for elevated eosinophilia levels were eight times more likely to experience intestinal strictures (abnormal narrowing) and liver disease (hepatic fibrosis) and were:
- Born earlier than other preemies.
- Born at lower birth weight than many preemies.
Complications and Long-Term Effects of NEC
Complications of NEC can include serious digestive problems, bowel obstruction, anemia, and neurological disabilities. The range and extent of long-term effects of NEC are dependent on any other medical complications related to premature birth the baby may be battling. Babies who undergo surgical correction of NEC face a 70% to 80% survival rate.
Causes of NEC
The causes of NEC are not clearly understood but a University of Iowa study published in 2009 described how incomplete development of a preemie’s blood capillary system results in inadequate nourishment to the mucosal cells developing in the immature digestive tract. Since babies are born without any gut bacteria to help with digestion, the Iowa study stresses the importance of oral feedings of human breast milk as soon as a preemie can take it. The study suggests the gut microbiome transferred from mother to baby via breast milk helps the baby’s digestive tract to mature more effectively and enables the baby to take in more nourishment sooner.
In 2012, the American Academy of Pediatrics issued an updated policy recommending preterm infants be fed human milk as soon as they are able to consume it. Previously, preemies were often not fed by mouth until after the 4th day of life in the hope of preventing NEC but current studies do not endorse this practice.
When mother’s or donor’s milk is unavailable, probiotics added to formula can help. Previous studies indicate breastfed preemies are less likely to develop NEC than formula-fed preemies.
Sources:
- Wahidi, L. S., et al. "Early Persistent Blood Eosinophilia in Necrotizing Enterocolitis Is a Predictor of Late Complications." Neonatology 108.2 (2015): 137-42. Karger Publishers. Web. 12 Oct. 2015.
- "New Predictor of Health Complications Can Identify High-Risk Preemies." MU School of Medicine. University of Missouri Health System, 30 Sept. 2015. Web. 12 Oct. 2015.
- "Necrotizing Enterocolitis." KidsHealth. The Nemours Foundation, n.d. Web. 12 Oct. 2015.