Umbilical Cord Blood Gases Normal Values
Labor & Delivery
Obie Editorial Team
Normal umbilical cord blood gas values
Median (5th-95th percentile): PH: 7.27 (7.12 – 7.35); pO2: 16.3 mmHg (6.2-27.6); PCO2: 55.1 mmHg (41.9-73.5); Bicarbonate: 24.3 mmol/L (18.8-28.2); Base excess: -3.00 mmol/L (-9.3 to +1.5); Lactate: 3.7 mmol/L (2.0-6.7)
What is the acid-base status
The intrapartum acid-base status, the status of the oxygen and other gases in the fetus and the umbilical cord after birth is important in establishing the link between events before and shortly after delivery. Analyzing cord blood gases (oxygen O2 and carbon dioxide CO2) from the umbilical artery is believed to be a good representation of the fetal acid-base status immediately before birth. Measurements of umbilical cord blood gases may be affected by several factors related to the method of sampling, storage, and assessment, and therefore there potentially a wide variation in accuracy.
Gas exchange between mother and fetus
All human beings including the fetus inside the uterus before birth depend on two gases, oxygen, and carbon dioxide are being exchanged, oxygen enters the body and carbon dioxide exits the body.
After birth, this exchange of gases happens in the lung, oxygen entering the body through inhaling and the lungs, and carbon dioxide leaving through exhaling and the lungs.
But before birth, the fetus does not use its lungs the same way we use after birth. The fetus does not breathe in the same way humans do outside the womb (although “chest movement or “practice breathing” do happen inside the uterus before birth).
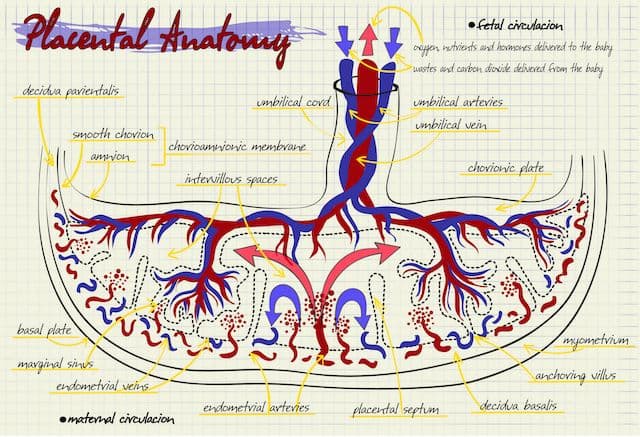
Instead, the exchange of gases, “breathing” occurs in the placenta where oxygen is transported from the mother's blood vessels into the placenta and then from the placenta through the umbilical cord to the fetus and carbon dioxide is exchanged from the fetus to the mother.
The placenta is an organ which is attached to the inside of the uterine wall and connects the fetus through the umbilical cord and allows for nutrient exchange, waste elimination and gas exchange via the mother’s blood supply.
Oxygenated blood from the mother diffuses into capillaries in the placenta and the vein into the umbilical cord, specifically into the umbilical vein, which picks up this oxygenated blood from the capillaries, and carries it to the baby’s heart, which pumps the blood throughout the baby’s body. Once the fetus uses this blood, it is carried away from the heart and back to the placenta by both umbilical arteries into the placenta and then to the mother.
In the intervillous space of the placenta, carbon dioxide diffuses from the fetus into the mother’s blood and the mother can eliminate it by exhalation through her lung. When she inhales, she picks up oxygen into her blood that is carried to the placenta and fetus.
What are umbilical cord blood vessels
There are 3 blood vessels in the umbilical cord connecting the fetus to and from the placenta: two arteries and one vein. The umbilical vein transports blood from the placenta/mother to the fetus and the two umbilical cord arteries carry blood back to the placenta/mother.
WHAT ARE UMBILICAL CORD BLOOD GASES
There are five different umbilical cord gases and other measurements that can be measured and calculated separately in the umbilical artery and the umbilical vein:
- Umbilical cord pO2 (oxygen)
- Umbilical cord pCO2
- Umbilical cord hCO3
- Umbilical cord pH
- Umbilical cord base excess or base deficit
Collecting umbilical cord blood gases
There are several steps involved in collecting umbilical blood cord gases:
- clamping a segment of the cord
- removing the clamped cord segment
- needle aspiration of two blood samples (one venous, one arterial) from the excised clamped cord segment into pre-heparinized syringes
The purpose of cord blood gas analysis is to determine the acid-base status of the neonate at the moment of delivery. Since acid-base status is in flux during the perinatal period, the timing of isolating a sample for analysis is crucial.
Immediately after birth, ideally before the baby’s first breath, an approximate 20-cm segment of the cord must be isolated between two sets of two clamps. Delay in clamping may result in significant change in acid-base parameters; the longer the delay, the greater is the change. The change is a progressive decrease in pH and base excess, and an increase in pCO2 and lactate.
What is the difference between the umbilical cord blood vein or artery
The blood in the umbilical vein reflects the placental condition. On the other hand, blood in the two umbilical arteries reflects the fetal status.
What affects umbilical cord blood gases values
There are maternal, uteroplacental, and fetal factors which can have an impact on umbilical cord blood gases.
Maternal factor
respiratory disease
hypoventilation,
seizure, trauma
smoking
Maternal reduced oxygen-carrying capability due to:
- anemia
- carboxy- hemoglobinemia
Decreased uterine blood flow due to:
hypotension (e.g.shock, sepsis)
regional anesthesia
maternal positioning
Chronic maternal conditions:
- diabetes
- chronic hypertension
- SLE
- antiphospholipid syndrome
Utero-placental factors
Excessive uterine activity
hyperstimulation
prolonged labor
placental abruption
Utero-placental dysfunction
placental abruption
placental infarction/dysfunction marked by intrauterine growth restriction, oligohydramnios or abnormal Doppler studies
chorioamnionitis (infection)
Fetal factors
Umbilical cord compression
oligohydramnios
cord prolapse or entanglement
Decreased fetal oxygen-carrying capability
significant anemia due to isoimmunization, maternal-fetal bleed or vasa previa
carboxy- hemoglobinemia (if the mother is a smoker)
Both umbilical cord blood venous or arterial values may be influenced by many different conditions including but not limited to:
- Labor itself: Labor itself can change umbilical blood gas values
- Medical conditions of the mother: These include hypertension, low blood pressure, diabetes, connective tissue conditions such as lupus and maternal lung problems.
- Length of labor: The length of labor may affect the umbilical cord blood values. At both extremes, too short labor and too long labor can impact umbilical cord blood gases.
- Delivery mode: The delivery mode, whether it's a cesarean or a vaginal birth can affect umbilical cord blood values.
- Cord anomalies: Most umbilical cord anomalies do not harm the baby. There are several known cord anomalies that can affect umbilical cord blood gas values including a knot in the cord, an umbilical cord twisted around the fetus' body parts (eg neck, limbs), a single umbilical artery, vasa previa, umbilical cord cysts.
- Cord prolapse:
- Placenta anomalies: Placenta previa, vasa previa
- Abruptio placentae: A detachment of the placenta can affect the gas exchange between the placenta and the mother and prevent gases to be exchanged between mother and fetus.
- Chorioamnionitis: An infection of the placenta and fetal membranes can affect the cord gases
- Congenital fetal anomaly: A baby with certain fetal anomalies can have abnormal cord gases
- Fetal anemia: Fetal anemia can affect the cord gases
- Fetal heart rate abnormalities: These can affect cord gases
- Instrument Deliveries: Studies have confirmed that instrumental deliveries such as with forceps or vacuum can affect blood gases.
- Meconium Aspiration: Meconium and meconium aspiration can affect cord gases
- Shoulder Dystocia: Shoulder dystocia can affect blood gases.
- Splenic Artery Aneurysm: This can affect blood gases
- Substance Abuse: Illegal drug use such as met or heroin can affect blood gases
- Twin B Delivery Problems: Second twins at vaginal births can have different blood gases
- Unclear: Many times, abnormal blood gases are difficult or impossible to explain.
- Uterine Rupture: A uterine rupture can affect blood gases
How to evaluate the fetal status
In order to examine the fetus' status, umbilical artery blood needs to be examined as this is the blood coming from the baby (as opposed blood going to the baby through the umbilical veins). If umbilical artery blood is abnormal, then causes should be considered.
WHAT ARE UMBILICAL CORD BLOOD GASES NORMAL VALUES
There are wide ranges of umbilical cord gas values which can be considered normal. But whether a value is normal or not depends often on the circumstances of the birth and other information.
Normal values of umbilical arterial samples in a preterm newborn:
Median and centile ranges for umbilical cord blood gas and lactate values
Median (5th-95th percentile)
- PH: 7.27 (7.12 – 7.35)
- pO2: 16.3 mmHg (6.2-27.6);
- PCO2: 55.1 mmHg (41.9-73.5)
- Bicarbonate: 24.3 mmol/L (18.8-28.2)
- Base excess: -3.00 mmol/L (-9.3 to +1.5)
- Lactate: 3.7 mmol/L (2.0-6.7)
*The “P” in PCO2 and PO2 stands for “partial pressure,” which is how these umbilical cord blood gases are measured.
White C, Doherty D, Henderson J et al. Benefits of introducing universal cord blood gas and lactate analysis into an obstetric unit. Australia and New Zealand J of Obstetrics and Gynaecology 2010; 50: 318-28









