Preventing Thyroid Disease During Pregnancy
Pregnancy News
Obie Editorial Team
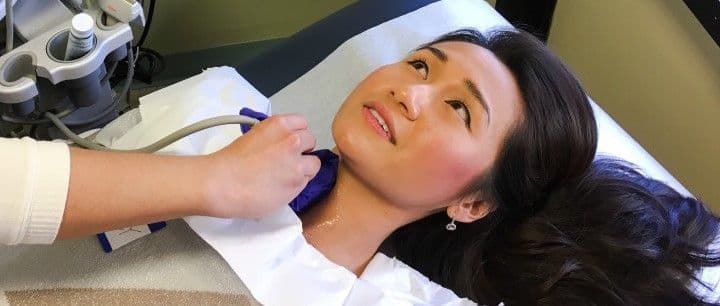
The findings of a clinical study showing the dangers of inadequate thyroid activity to a pregnant woman’s health, and that of her unborn child, have compelled an American Thyroid Association (ATA) task force to put together new clinical guidelines. The guidelines launched in the journal Thyroid, focused on the prevention and regulation of thyroid disease in pregnancy.
Clinical researchers have shown that hyperthyroidism, hypothyroidism and subclinical thyroid disorders have dangerous effects on pregnant women and the cerebral development of the fetus. Ongoing studies show the connection of miscarriage and premature delivery in pregnant women with regular thyroid functions but are positive for thyroid peroxidase antibodies. The studies further revealed that postpartum thyroiditis have long-lasting effects.
A panel of international experts in the fields of obstetrics/gynaecology, endocrinology, and nurse midwives helped develop the new guidelines. The new clinical rules concentrate on several areas in the diagnosis and regulation of thyroid disease during pregnancy and postpartum period. These include thyroid functionality tests, postpartum, postpartum thyroiditis and hypothyroidism. Additional areas focused on were miscarriage and preterm delivery, thyrotoxicosis, thyroid nodules, thyroid antibodies, suggestions for thyroid disease screening for pregnant women and other areas beneficial to upcoming research.
The new set of guidelines recommends oral levothyroxine treatment to women with thyroid disorders like overt hypothyroidism or subclinical hypothyroidism who are positive for the TPO antibody. Using triiodothyronine (T3) and desiccated thyroid preparation in the treatment of maternal hypothyroidism are not recommended. One of the specific recommendations presented in the new guidelines is pregnant women who have subclinical hypothyroidism but were not treated to begin with need to be observed for possible development to overt hypothyroidism by using serum TSH as well as free T4 measurements once every 4 weeks up until the 16 to 20 weeks gestation and be tested at least one time around 26 to 32 weeks gestation.
Thyroid disease in pregnant women is not unheard of. Pregnancy has some effect on the thyroid gland and its functions. This is why women who have iodine deficiency or limited thyroidal reserve will most likely be affected with hypothyroidism. A pregnant woman who develops hypothyroidism has high risks of having miscarriage. The disease can also cause serious problems to the unborn child. Hypothyroidism can also develop after giving birth so the mother’s health needs to be monitored. The new ATA Guidelines will be disseminated extensively to improve patient care, set up ideal care and protection of the pregnant women and her baby and direct more research to further understand the disease.
Source: Thyroid. Alex Stagnaro-Green, Marcos Abalovich, Erik Alexander, Fereidoun Azizi, Jorge Mestman, Roberto Negro, Angelita Nixon, Elizabeth N. Pearce, Offie P. Soldin, Scott Sullivan, Wilmar Wiersinga. 25 July, 2011.
Read More









_0.jpg&w=3840&q=75&dpl=dpl_Mp2bNUgprsMgwui5dCv43WVBEHKo)
