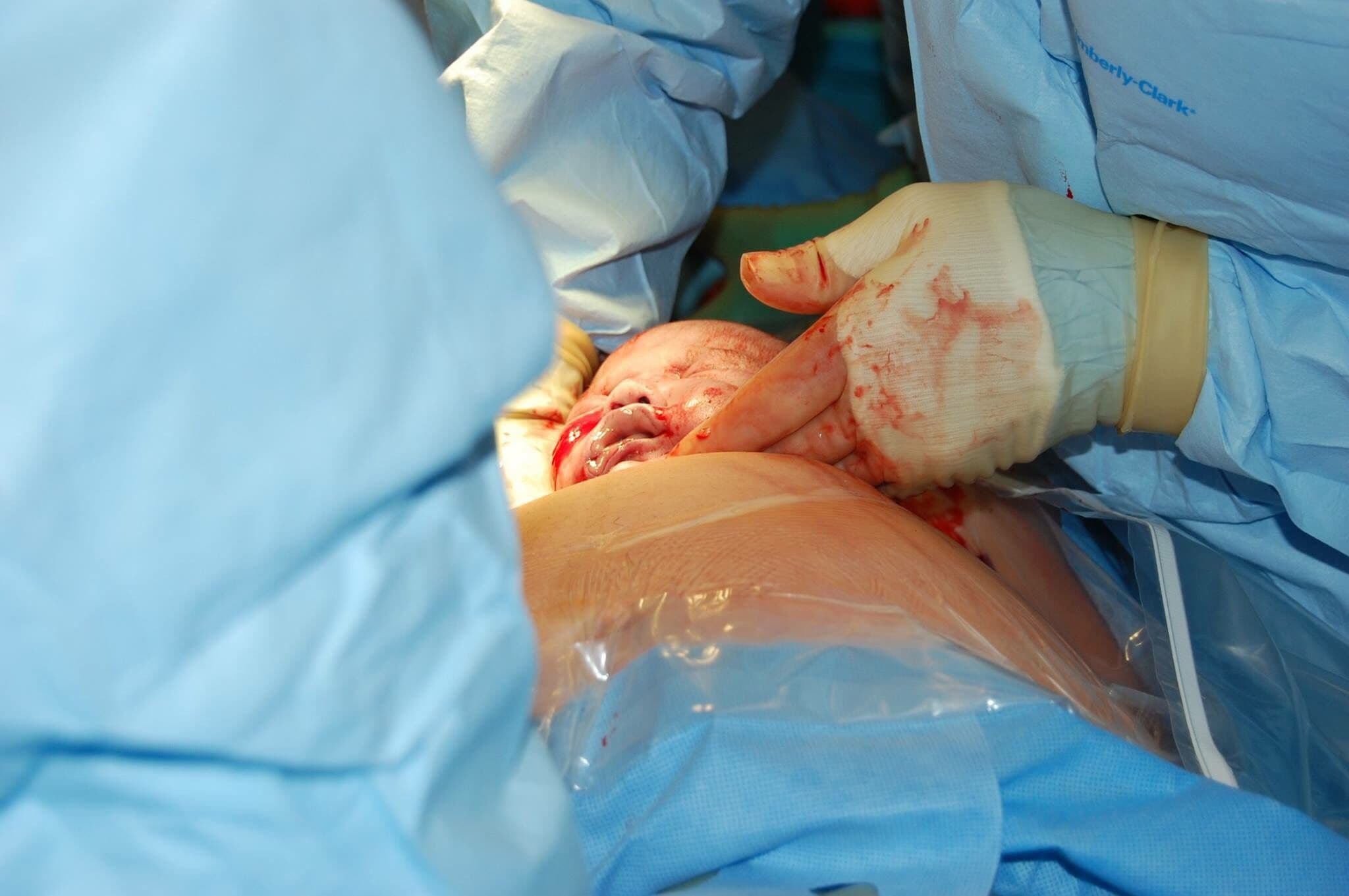
Repeat C-Sections and Uterine Rupture Risk
Pregnancy News
Obie Editorial Team

When we talk about pregnancy and childbirth, it's essential to understand the dynamic changes occurring within your body. The uterus is a remarkable organ that stretches to house and nurture your growing baby, and then returns to its regular size after a natural birth. However, when a C-section is performed, a surgical incision is made in the uterine wall. As this incision heals, it forms a scar, potentially affecting the uterus’s elasticity in future pregnancies. Scientific research has shown that such scars not only reduce the flexibility of the uterine tissue at the incision site but may also increase the risk of uterine rupture.
Evidence from the UK Obstetric Surveillance System indicates that the risk of uterine rupture tends to increase with each subsequent C-section. According to their findings, published in PLoS Medicine, other factors that might amplify this risk include shorter intervals between pregnancies and induced labor. Armed with this information, you and your healthcare provider can make informed decisions about managing future pregnancies and delivery methods.
What is Uterine Rupture and How Can It Be Avoided?
Uterine rupture is a rare but serious complication where the uterus tears, typically occurring during labor. This situation arises as the womb contracts to help position the baby for birth. When there are existing incision scars with less flexible tissue, there's a risk that contractions could stress these scarred areas, leading to a rupture. Awareness of this possibility allows healthcare teams to monitor and support you closely, providing interventions to minimize risks and prioritizing your safety and that of your baby. Prompt and attentive prenatal care is key here.
In a study involving nearly 160 women, with approximately 140 having had prior C-sections, the incidence of uterine rupture was low—specifically 0.2 in 1000. It's worth noting, though, that those with multiple prior C-sections had a higher incidence of ruptures. Tragically, in this study, two women lost their lives due to uterine rupture, and 18 infants passed away shortly after birth.
This vital evidence supports the notion that medical teams need to keep a diligent outlook for women with a history of C-sections, tailoring care for your unique situation. Your healthcare provider can help map out a personalized birth plan that proactively manages and mitigates these potential risks, ensuring you feel informed and empowered throughout your journey.
Source: KE Fitzpatrick, JJ Kurinczuk, Z Alfirevic, P Spark, P Brocklehurst, et al. PLoS Medicine. 15 March 2012.
Read More